Deaths Are An Incomplete Measure Of Covid-19’S Impact
Accompanying the pandemic of Covid-19 infections is also an “infodemic” of inaccurate, sometimes dangerous misinformation. Based on some of the claims by people who downplay or doubt the severity of the pandemic, it might be reasonable to conclude that the outbreak is no worse influenza in a bad year. Some even maintain that Covid-19 is less a concern than flu, and cite the pandemics of 1917-1918 and 1968 as evidence. Central to these opinions is a perceived overall low death rate, especially among younger people. It is not unusual to see attempts to trivialize the damage of this calamitous pandemic with comments such as “99.9% of people with Covid-19 survive!” or “It’s mainly the elderly and infirm who die.”
Even if true, claims like this are dangerously misleading. They paint a false picture, by focusing only upon the death rate without taking into consideration the outcome in survivors. It is here where Covid-19 and flu diverge and the already-faulty comparison of the two infections breaks down entirely.
Covid-19 is far more than a transient respiratory infection. Although it shares some pulmonary symptoms with influenza, for example severe pneumonia and a fever, once flu is gone, it’s gone and rarely leaves permanent damage. Not so with Covid-19. For example, “post-Covid pulmonary fibrosis” leaves permanent damage in the lungs, presumably resulting from blood clotting in the lungs. And it doesn’t stop there.
Influenza is an infection of the respiratory system, while the SARS-CoV-2 virus, the cause of Covid-19, attacks a long (and growing) list of other tissues in the body. In addition, there have been numerous reports of non-respiratory manifestations, such as loss of sense of smell or taste. This symptom is now so specific to coronavirus infection that is sometimes used to diagnose it. Covid-19 also often affects the brain and central nervous system. This leads to neurological symptoms, including confusion and cognitive impairments, fainting, sudden muscle weakness or paralysis, seizures, and ischemic strokes. Also, children can (quite rarely) develop a life-threatening malfunction of the immune system called Multisystem Inflammatory Syndrome (MIS-C), which presents with symptoms similar to Kawasaki disease.
The virus also can attack the digestive system; nausea, vomiting, and diarrhea are not uncommon, especially in younger people.
Kidney damage, an inherently unlikely symptom for a respiratory infection, may also occur; the death rate of Covid-19 patients on dialysis is disturbingly high. Some experts are predicting that an epidemic of kidney failure is likely in the near future.
For those who survive, recovery is often incomplete, with various symptoms persisting after the acute infection has subsided. A recent article in JAMA found that 87.4% of patients who had recovered from Covid-19 reported persistence of at least one symptom, most often fatigue or dyspnea (i.e., shortness of breath) two months after recovery. The frequency of post-acute Covid-19 symptoms is shown below:
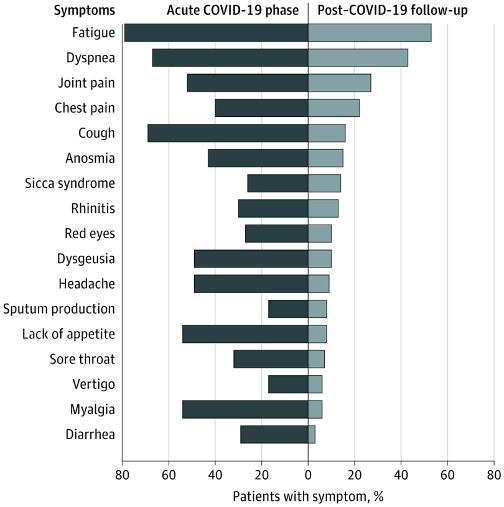
Source: https://jamanetwork.com/journals/jama/fullarticle/2768351?appId=scweb
The finding that almost nine in 10 of people who had recovered from Covid-19 reported persistence of at least one symptom two months later, illustrates the flaw in focusing solely on fatality rates.
Particularly worrisome are the numerous reports of patients experiencing long-term adverse effects that resemble a condition variously known as myalgic encephalomyelitis or chronic fatigue syndrome (ME/CFS). Its signs and symptoms may include fatigue, loss of memory or concentration, sore throat, swelling of neck or armpit lymph nodes, unexplained muscle or joint pain, headaches, non-restorative sleep, and extreme exhaustion that lasts more than 24 hours after physical exercise or mental stimulation (“post-exertional malaise”).
People with ME/CFS are often incapable of performing ordinary activities, and sometimes become completely debilitated, unable even to get out of bed. A good word picture was provided in an interview of three Covid-19 patients on NPR’s July 11 “Weekend Edition,” who described in poignant terms their ongoing symptoms, and CNN anchor Chris Cuomo recently described on-air his experience with some of these symptoms following his bout with Covid-19. The manifestations of ME/CFS can persist for years, although, of course, we can’t yet know what the typical, long-term post-Covid-19 course will be.
The appearance of serious, persistent Covid-19 sequelae has important implications.
First, we need to aggressively suppress and mitigate Covid-19. The fewer new cases, the fewer lingering illnesses there will be, with all their attendant misery and expense. (A corollary is that “Covid parties” are dangerous, antisocial, and colossally stupid.)
Second, the persistence of debilitating symptoms calls into question the wisdom of vaccine “challenge trials,” in which infectious SARS-CoV-2 virus is intentionally administered to test subjects, some of whom have received a trial vaccine while others a placebo. In the absence of highly effective drugs to treat Covid-19, such studies are arguably unethical.
Finally, we need research on the long-term effects of Covid-19, so that we can better understand the pathophysiology of both the acute viral infection and the persistent post-infection sequelae. A research group at the NIH’s National Institute for Neurological Diseases and Stroke is preparing to enroll patients in a study that will investigate possible aberrations in the immune systems of “long-haulers,” people who have persistent symptoms after recovering from Covid-19, but we need much more.
It is clear that Covid-19 is a complex and dangerous infection. Simple statistics like the number of deaths or death rates don’t even begin to tell the whole story.
Read More
